Groin skin irritation is far more common than most people are willing to acknowledge, largely because it affects an intimate area that many feel uncomfortable discussing openly. Yet the groin is uniquely vulnerable. Constant movement, skin-on-skin friction, warmth, and moisture create conditions that challenge even healthy skin. Early signs often appear subtly: mild itching, tightness, sensitivity, or faint redness that seems easy to dismiss. Over time, these signals can intensify into persistent discomfort that interferes with daily routines. Walking, exercising, working long hours seated, or even sleeping may become irritating rather than effortless. Many people mistakenly assume these symptoms reflect poor hygiene, but the reality is far more nuanced. Even individuals with excellent hygiene can experience irritation when the skin’s protective barrier becomes compromised. Sweat trapped against the skin creates an environment that promotes inflammation, while repeated friction from clothing steadily weakens the surface layer. The groin’s high concentration of hair follicles also increases susceptibility to ingrown hairs and follicular inflammation. Recognizing these early symptoms as physiological signals rather than personal shortcomings is the first step toward effective care and long-term prevention.
One of the most common contributors to groin irritation is ingrown hair, which occurs when hair curls back into the skin instead of growing outward. This is especially likely after shaving or waxing, particularly when hair is coarse or curly. The skin responds with redness, itching, tenderness, and small raised bumps that can resemble acne. In some cases, these bumps may become infected, leading to swelling or pus. Tight clothing exacerbates the issue by pressing hair back into the skin and increasing friction throughout the day. Closely related is folliculitis, a condition involving inflammation of the hair follicles themselves. Folliculitis can be triggered by bacteria, fungi, sweat, or mechanical irritation and often appears as clusters of red or white-headed bumps that may feel itchy, sore, or sensitive. People who exercise frequently, sweat heavily, or wear non-breathable fabrics are at higher risk. While mild cases may resolve with rest and gentle care, persistent folliculitis can spread and worsen without attention. Understanding these conditions helps reduce unnecessary anxiety while guiding more effective responses, such as moderating hair removal practices and giving the skin adequate time to recover.
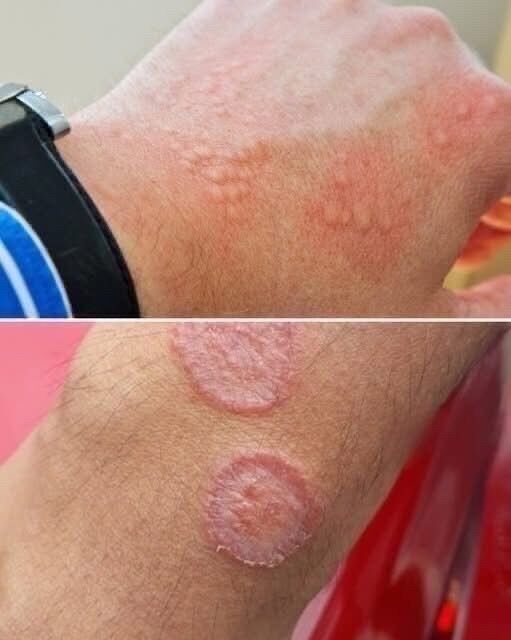
Fungal infections are another significant cause of groin irritation, with tinea cruris, commonly known as jock itch, being among the most prevalent. Fungi thrive in warm, damp environments, making the groin particularly susceptible. Jock itch often begins as an itchy, red patch that gradually spreads outward, sometimes forming a scaly or sharply defined border. Unlike simple chafing, fungal infections tend to persist and may worsen without treatment. Although men are more frequently affected, anyone can develop this condition, especially in hot climates or during periods of heavy sweating. Shared locker rooms, communal showers, damp towels, and wearing moist clothing for extended periods increase exposure and risk. Many people initially mistake fungal irritation for simple friction-related discomfort and delay treatment, allowing the infection to become more established. Effective management includes keeping the area clean and thoroughly dry, changing out of sweaty clothing promptly, and using antifungal treatments consistently for the full recommended duration. Early awareness and intervention not only speed recovery but also reduce the likelihood of recurrence or spread to other areas of the body.
Allergic and irritant reactions also play a substantial role in groin skin problems, often classified under contact dermatitis. This occurs when sensitive skin reacts to substances such as scented soaps, body washes, laundry detergents, fabric dyes, or personal care products. The groin is more reactive than many other areas of the body, meaning products tolerated elsewhere may cause redness, itching, or burning here. Symptoms can develop suddenly or gradually, depending on exposure. Another related condition is intertrigo, which arises in skin folds where heat, moisture, and friction coexist. Intertrigo presents as red, inflamed, sometimes raw-looking skin that may sting or develop an unpleasant odor, particularly if a secondary infection occurs. Individuals who are physically active, live in humid climates, or experience frequent sweating may encounter this condition more often. Managing these issues requires reducing moisture, eliminating irritants, and allowing the skin to breathe. Switching to fragrance-free products, wearing breathable fabrics, and prioritizing airflow can significantly improve symptoms over time.
Prevention and daily care play a critical role in minimizing groin irritation and supporting long-term skin health. Hygiene is important, but excessive washing or harsh cleansers can strip away natural oils that protect the skin barrier. Gentle cleansing with mild, unscented products is usually sufficient. Thorough drying after bathing, sweating, or swimming is equally essential, as lingering moisture encourages irritation and infection. Clothing choices matter more than many realize. Loose-fitting garments made from breathable materials reduce friction and allow heat and moisture to dissipate. When hair removal is part of personal grooming, spacing out sessions, using clean tools, and avoiding extremely close shaving can reduce the risk of ingrown hairs and folliculitis. For those prone to fungal issues, preventive antifungal powders or creams may be helpful during high-risk periods. These consistent, preventative habits often have a greater long-term impact than reactive treatments used only once discomfort becomes severe.
Knowing when to seek medical guidance is an important aspect of managing groin skin concerns. While many cases improve with attentive self-care, persistent or worsening symptoms should not be ignored. Spreading redness, increasing pain, swelling, discharge, or fever may indicate infection requiring professional treatment. Recurrent irritation may signal underlying factors such as chronic skin sensitivity, metabolic conditions, or immune-related issues that deserve evaluation. Consulting a healthcare professional can provide clarity, targeted treatment, and reassurance. Ultimately, understanding groin skin irritation empowers individuals to respond early, care for their bodies with confidence, and reduce unnecessary discomfort. By viewing these issues as common health concerns rather than sources of embarrassment, it becomes easier to maintain comfort, dignity, and long-term well-being in everyday life.